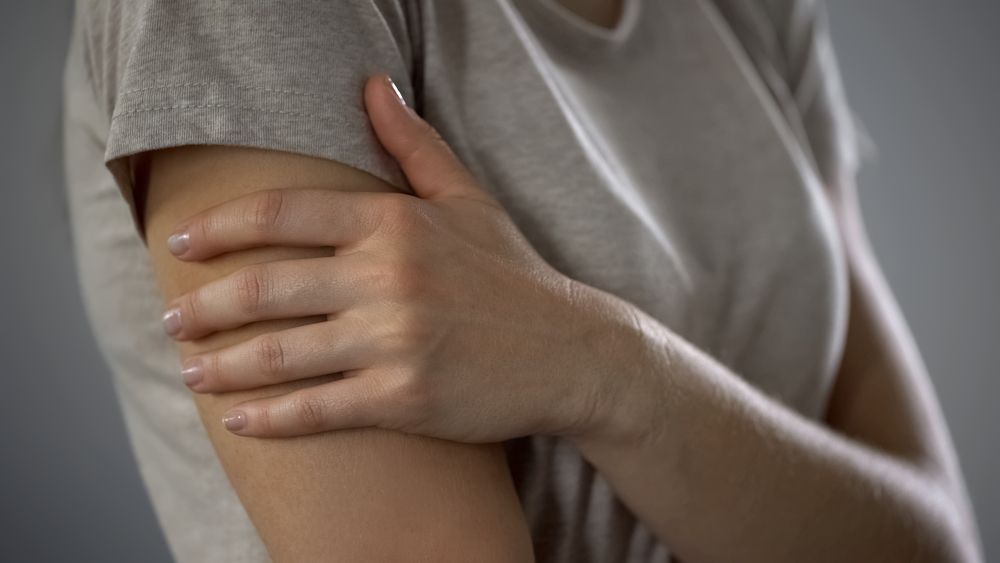
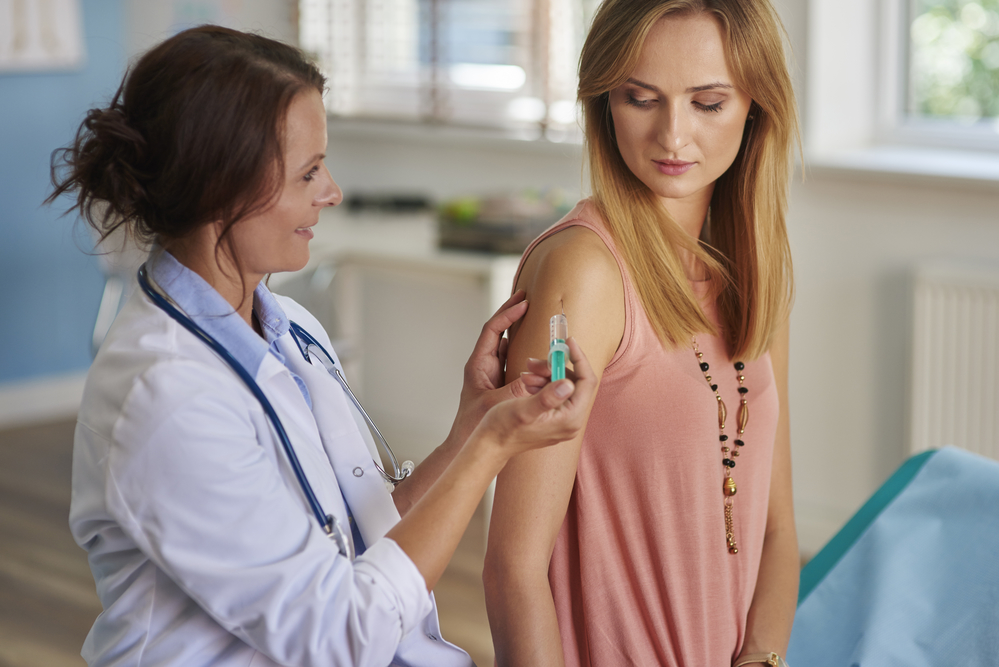
There have been several measles outbreaks internationally including in Sydney, of late. Nearly 100 cases have been reported for 2019 so far this year, which is not far from the total number of people for the whole of 2018 according to the Dept. Health.
The common question therefore is, am I protected and should I get a booster?
The answer is, if you were born before 1957, the recommendation is that you would have been exposed and it is therefore not necessary, and if you were born after 1957 – it depends!
If you’ve ever had measles, you don’t need a vaccination.
If you’ve had 2 doses of the vaccine (this started generally after the 1980s), then it is not necessary.
If you’ve only had 1 dose then a booster should be considered.
If you’re not sure, we can check your antibody status with a simple blood test.
It’s also useful to note that it generally takes 2-4 weeks for a person to develop protective antibody levels after the vaccine. An infected person will usually spread it to 18 others, assuming the others are unvaccinated.
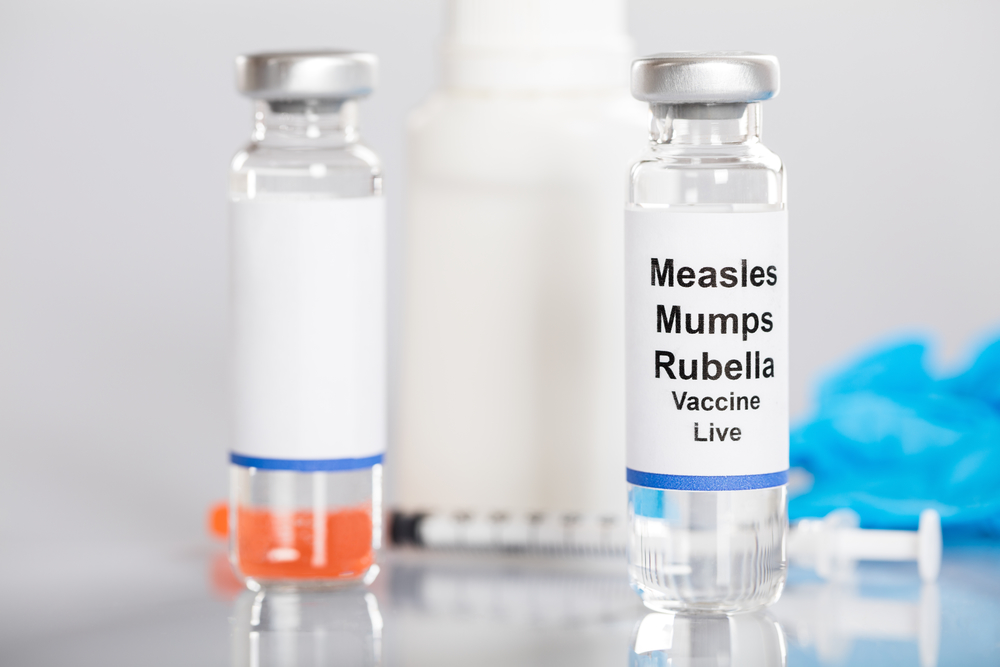
What are the risks of measles?
Generally speaking, pregnant women are at high risk as are infants. Rarely, an inflammatory brain condition called subacute sclerosing panencephalitis can occur, through complications, a decade or so after a child has their primary infection. Measles can also cause deafness, particularly in children.
The symptoms are: fever, sore eyes, cough, followed by red blotchy rash on the head and neck that spreads to the rest of the body.
The measles vaccine is free for anyone born during or after 1966 who hasn’t already had 2 doses.
The antivaxxers would argue that there are complications to vaccinations e.g. autism. A major recent Danish study showed that the MMR vaccine did not increase the risk of autism or trigger autism in susceptible children and wasn’t linked with clustering of autism cases following vaccination.
What about other vaccines?
For those over the age of 65, we would recommend a pneumococcal vaccine. This vaccinates against the pneumococcal bacteria which is responsible for 20% of bacterial pneumonias. This is a vaccine that is given every 5 years, and the reason for starting to consider this at age 65 is due to the fact that at this age, one’s natural immunity starts to waive as part of ageing.
A shingles vaccine can also be considered. This is a one-off vaccine that protects against the reactivation of the chicken pox virus (if you’ve had chicken pox), and gives up to 60% efficiency for prevention of the outbreak of shingles. Shingles can be debilitating in the long term with neuropathic pain or Itch Syndrome, and if it occurs in the eye, it can cause significant eye complications. The cardinal manifestation is a blistering rash generally in a linear distribution that follows a nerve. The distribution is often preceded by a program of itch or tingling several days beforehand.
Tetanus should be given as a booster every 10 years.
Some adults also request a whooping cough and/ or diphtheria booster as they are soon to be grandparents and clearly don’t wish to infect their infant grandchildren.
If you have any concerns or would like to get your antibody status checked, please book in a time with our team here.